Introduction
Femoral shaft fractures are among the most common pediatric orthopedic injuries and represent a leading cause of hospitalization for orthopedic trauma in children. The annual incidence of femoral shaft fractures in children has been estimated at 19 per 100,000 (Hinton et al. 1999). Standard treatment for these fractures in patients aged six months to five years involves fracture reduction followed by immobilization with a hip spica cast (Wright 2000). Early application of hip spica casting has been associated with shorter hospital stays and a lower risk of malunion compared to prolonged traction (Rasool, Govender, and Naidoo 1989).
Pain management in pediatric femoral shaft fractures is commonly achieved through a multimodal approach, with both oral and intravenous (IV) opioids frequently utilized. However, opioid use carries significant immediate and long-term risks, including respiratory depression, dependence, and potential neurodevelopmental consequences (Jones et al. 2021). Orthopedic surgeons account for one of the highest rates of opioid prescriptions across all age groups, with some studies suggesting orthopedic providers contributing to approximately 8% of all opioid prescriptions in the United States (Hudgins et al. 2019; Volkow et al. 2011). Current clinical guidelines advocate for a multimodal pain management strategy to reduce opioid consumption while ensuring adequate analgesia (Chou, Gordon, de Leon-Casasola, et al. 2016). This is particularly important, as the age of initial medical opioid use has been linked to an increased risk of future misuse and abuse (Miech et al. 2015).
Prior studies have demonstrated that femoral nerve blockade in children with femoral shaft fractures results in significant pain reduction (Ronchi et al. 1989). Although effective, regional nerve blockade carries risks, including potential nerve injury, local anesthetic systemic toxicity, and technical challenges in pediatric patients. Hematoma blocks, involving the direct application of local anesthetics to the fracture site, have shown promise as an adjunctive technique for pain management. One study by Herrera et al in 2004 looked at their use in elastic nailing of pediatric femoral shaft fractures and demonstrated an increase in time to use of initial narcotic dose after surgery, with minimal to no adverse effects. This study also demonstrated a trend in decreased total narcotic usage, however this difference was found to be statistically insignificant with a small cohort size (Herrera, Wall, and Foad 2004). Another study recently published by Yue et al in 2023 looking at the use of hematoma blocks in adult femoral shaft fractures treated with intramedullary nailing demonstrated a reduction in both pain scores and perioperative opioid consumption (Yue et al. 2023). The AAOS 2020 Clinical Practice Guidelines for Treatment of Pediatric Diaphyseal Femur Fractures gives a two-star limited recommendation for use of regional pain management based off some of these studies (American Academy of Orthopaedic Surgeons 2020). However, to our knowledge, no specific study has examined the use of hematoma blocks in pediatric femoral shaft fractures treated with spica casting.
This study aims to evaluate the effectiveness of hematoma blocks in controlling pain and reducing opioid consumption in pediatric patients with femoral shaft fractures treated with hip spica casts. Our study also aims to serve as a pilot study to help determine the feasibility of a multi-center randomized control trial examining the efficacy of hematoma blocks in spica casting with a larger cohort and higher level of evidence. Our primary outcome measure is the 24-hour perioperative opioid consumption. Secondary outcomes included perioperative complications, operative timing and fracture healing.
Methods
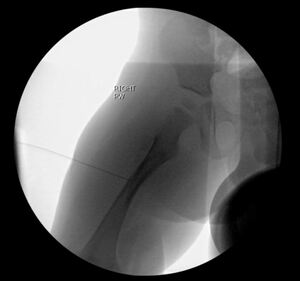
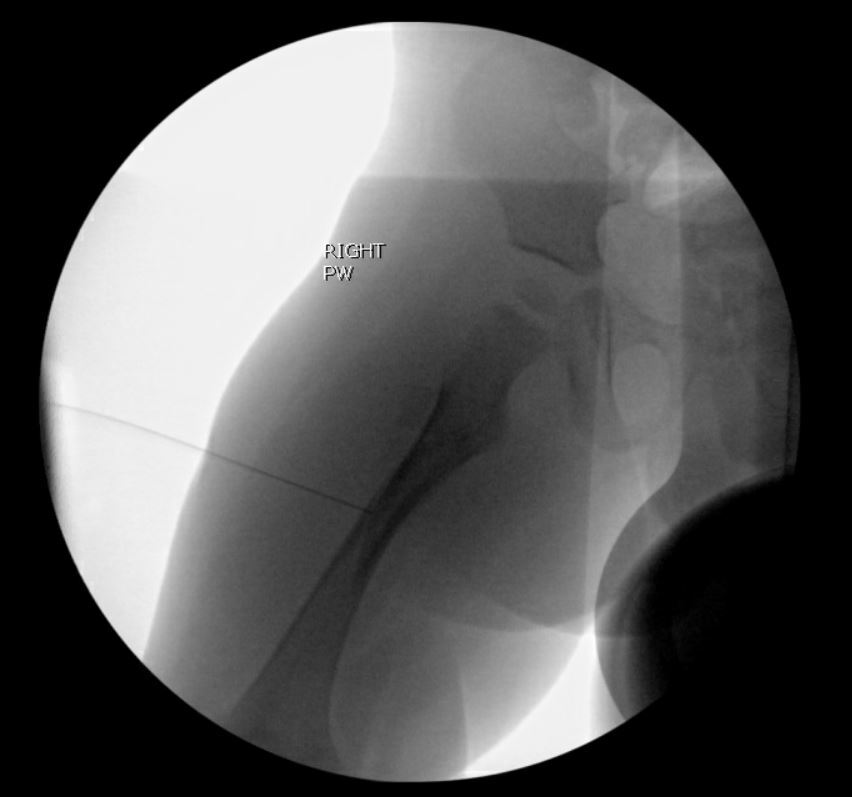
We conducted a retrospective cohort study including pediatric patients treated for femoral shaft fractures with hip spica casting between 2018 and 2020 by three different fellowship trained pediatric orthopedic surgeons at the institution. Patients either received a hematoma block intra-operatively or not based on provider preference and were retrospectively divided into two groups: those who received a hematoma block in the operating room (OR) (n=20) and those who did not (n=15). Hematoma blocks were administered using local anesthetic injection at the fracture site before cast application. A 10mL volume of 0.2% ropivacaine was injected into the fracture hematoma using a lateral based approach under fluoroscopic guidance (Fig 1).
24-hour perioperative narcotic pain medication administration was recorded in three phases of care across all groups: intra-operative, post-operative in the PACU, and post-operative on the floor. Narcotic pain medications used included IV fentanyl, oral solution oxycodone and oral solution hydrocodone-acetaminophen. All patients underwent general anesthesia for the procedure with IV sedation. All patients had oral solution ibuprofen administered in the immediate post-operative period as a first line agent for multi-modal pain control. There was no standardized protocol for perioperative pain medication management with the decision to administer medications based on subjective pain assessments intra-op and post-op left to the discretion of the anesthesiologist and nursing staff.
Age, sex, laterality, fracture pattern, time in OR, length of stay, fracture union rates, complications and morphine equivalent doses were recorded for all patients in this study. The primary outcome measure was opioid consumption over a 24-hour perioperative period, quantified in morphine milligram equivalents (MME). Statistical analysis was performed using the Mann-Whitney U test to compare differences in 24-hour MME usage between the two groups and t-test and chi-squared test to analyze differences in patient demographics. Statistical significance was set at p<0.05. Ethical approval for the study was obtained from the institutional review board, and informed consent was secured from the guardians of all participants.
Results
A total of 35 pediatric patients were included in the study, divided into two groups: 20 in the hematoma block group and 15 in the non-hematoma block group. The demographics of the cohort are described in Table 1 with no statistically significant differences when looking at age and sex (Table 1).
The hematoma block group had an average procedure time that was 5.77 minutes longer (31.9 vs 26.13 minutes, p = 0.046) than the non-hematoma block group. The hematoma block group had an average length of stay, based on discharge on post op day zero (POD0) or post op day one (POD1), that was 0.18 days shorter but not statistically significant (0.35 vs. 0.53, p = 0.296). Perioperative opioid consumption over 24 hours was lower in the hematoma block group, though this difference was small and not statistically significant (2.51 vs 2.71, p = 0.76). When couched in terms of weight-based dosing, there was no difference in 24-hour MME usage between the two groups (0.18 vs 0.18, p = 1.0) (Table 2).
All patients demonstrated radiographic union by three months. One patient in the hematoma block group required return to the operating room for open reduction and internal fixation after a loss of reduction in the spica cast at the 2-week follow-up.
Discussion
Previous studies have demonstrated improvements in pain control using intra-operative hematoma blocks in pediatric femur fractures treated with elastic nail fixation. The AAOS 2020 guidelines provide a “limited” recommendation for their use in perioperative pain management. The study in 2004 by Hererra et al. referenced in the AAOS guidelines found a statistically significant increase in time to first narcotic administration in their hematoma block group, however while there was a trend toward lower MME usage, this was not found to be statistically significant, with the study limited by its small sample size (Herrera, Wall, and Foad 2004). To our knowledge, this is the first study specifically evaluating the use of hematoma blocks in pediatric patients with diaphyseal femur fractures treated with spica casting.
Our findings suggest that the use of an intra-operative hematoma block can reduce post-operative opioid consumption for pediatric femur fractures treated with spica casting. However the trend toward lower MME usage in the hematoma block group was not statistically significant, and no difference was observed when accounting for weight-based dosing.
There were no complications associated with the hematoma block. However, the procedure time was significantly longer in the hematoma block group, with an average increase of 5.77 minutes. While this increase may not have clinical significance, it is important to minimize operating room time and anesthesia exposure, which are key considerations in patient care. Interestingly, in similar studies by Hererra et al. and Yue et al., procedure times in the hematoma block groups were 28 and 1.2 minutes shorter, respectively (Herrera, Wall, and Foad 2004; Yue et al. 2023). They postulated that the difference in procedure time was most likely due to the procedures being performed by different surgeons between study groups, which likely played a role in this study as well.
Several limitations affected our study. The small sample size of 35 patients limits the generalizability of our findings. A post-hoc power analysis indicated that a sample size of 300 patients would be required to detect a statistically significant difference in MME usage. Notably, the lack of a standardized post-operative pain management protocol posed a challenge. Patients received various narcotic medications, and assessing pain in pediatric patients is inherently difficult, with post-operative narcotic administration based on nursing discretion in the PACU and on the floor.
Given the trend in reducing post-operative opioid consumption, we believe our pilot study does validate the feasibility of a larger multi-center study. Future studies should aim for larger cohorts and a standardized post-operative pain management protocol to more accurately assess the efficacy of intra-operative hematoma blocks for pediatric diaphyseal femur fractures treated with spica casting.
Patient Consent
The author(s) declare that no patient consent was necessary as no images with identifying information are included in the article.
IRB Approval
This study was reviewed by The Legacy Emanuel Institutional Review Board, and based on the information provided, the IRB determined that this study meets the criteria for Exempt Status in accordance with federal regulations at 45 CFR 46.104.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Declaration of Competing Interests
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.