Introduction
Chronic patellar tendinosis, also known as Jumper’s Knee, is a tendinopathy syndrome due to chronic degeneration of the patellar tendon (Blazina et al. 1973; Dan et al. 2019). The syndrome is typically characterized by pain and tenderness of the inferior pole of the patella and the proximal part of the patellar tendon, which may lead to functional impairment in athletes and non-athletes alike (Brockmeyer et al. 2015; Villardi et al. 2019; De Vries et al. 2017). Incidence of patellar tendinopathy is 14-17% in the general population, and 32-44% for individuals engaged in high-impact activities such as basketball, volleyball, dancing, running, soccer, and rugby (Andriolo et al. 2019; Lian, Engebresten, and Bahr 2005). While many cases may heal spontaneously, the degree of pain or functional limitation may cause early termination of an athlete’s career, with as many as 20% of cases becoming recalcitrant (Villardi et al. 2019; Andriolo et al. 2019; Ferretti et al. 2002; Kaeding, Pedroza, and Powers 2007).
Jumper’s Knee can be classified into four classes using the Blazina scale to rate the severity of symptoms (Blazina et al. 1973). Grades I and II are often successfully treated with conservative management such as non-steroidal anti-inflammatory (NSAID) medications, rest or activity restriction, cryotherapy, shock-wave therapy, and physical therapy with an eccentric-loading focus (Andriolo et al. 2019; López-Royo et al. 2020). The latest research shows that dry needling, percutaneous electrolysis, transverse friction massage, stretching, and squatting on inclined planes may also be effective at treating milder cases (Ragone et al. 2024). If persistent, minimally invasive treatments include platelet-rich plasma (PRP), polidocanol, and aprotinin injections, or injection of autologous skin derived tendon-like cells and bone marrow mononuclear cells (Andriolo et al. 2019; López-Royo et al. 2020). Failure of conservative management for three-six months often leads physicians and patients to pursue surgical intervention.
Surgical options for refractory patellar tendinosis include both open and arthroscopic approaches (Brockmeyer et al. 2015; Lee et al. 2018; Rodriguez-Merchan 2013). Open procedures may involve drilling or resecting the distal patella, microvascular reinforcement, longitudinal incisions through the patellar tendon, closing of the paratenon, or surgical tendon stimulation. Arthroscopic procedures may involve shaving the dorsal side of the proximal tendon, debridement of the Hoffa’s fat pad, osteoplasty and removing hypertrophic synovitis around the inferior patellar pole, tendon debridement, or denervation/cauterization of peri-patellar vessels and nerves (Brockmeyer et al. 2015; Kaeding, Pedroza, and Powers 2007; Rodriguez-Merchan 2013; Romeo and Larson 1999).
There is a paucity of literature about the factors predicting success and improved functional scores in arthroscopic debridement of chronic patellar tendinosis. The decision to perform bony work on the patella or not is still a topic of debate (Brockmeyer et al. 2015; Kaeding, Pedroza, and Powers 2007). The same holds true for soft tissue practices such as Hoffa’s fat pad debridement or denervation of the inferior patellar pole (Brockmeyer et al. 2015). The purpose of this study is to improve understanding of which perioperative variables may influence outcomes and return to activity after arthroscopic debridement of patellar tendinopathy. The current hypothesis is that arthroscopic surgical debridement with patellar bony work, Hoffa’s fat pad debridement, denervation and cauterization of hypertrophic vessels, and early post-operative mobilization results in clinically significant improvement in pain and promotes return to baseline activity after two years of follow up with proper post-operative rehabilitation.
Methods
Study Selection
A systematic review of the literature was conducted through Pubmed, CINAHL, Cochrane, and Embase databases using the search terms outlined in Appendix Table 1. The final literature search was conducted in March 2024, including any papers published since 2000 in an effort to find sufficient studies meeting inclusion criteria while remaining as contemporary as possible. In total, 1885 results were screened. After 201 duplicate studies were removed, 1684 studies were screened against title and abstract using PRISMA guidelines (Moher et al. 2010). 1601 studies were excluded leaving 83 studies to be assessed for full-text eligibility against the inclusion criteria. Study selection is summarized in Figure 1. Additional studies were manually searched for during review of study references, but none were included.
Inclusion and exclusion criteria are summarized in Table 1. Prospective of Level IV or higher evidence published in English between January, 2000 and the search date of March, 2024 were included. Study participants must have been diagnosed and treated arthroscopically for patellar tendinopathy. Studies must have compared either two different surgical techniques, surgery to placebo surgery, surgery to exercise, surgery to nonsurgical modalities, or measured study outcomes before and after surgery. All of this is to assess of the success of arthroscopic procedures (in relation to other surgical modalities or non-surgical management) and to identify the factors mitigating their success. All studies must have measured knee pain and/or function by standardized scale: Visual analog scale (VAS), Marx activity rating scale, Victorian Institute of Sports Assessment patellar tendon (VISA-P), Tegner activity scale (TAS), Lysholm rating scale, International Knee Documentation Committee (IKDC), or other Quality of life (QOL) scores, and must have had a mean follow-up of six months or greater. These authors believed that a six month follow-up would be robust to capture a breadth of post-operative outcomes with some outcomes, like return to sport, requiring at least three months after patellar tendinopathy surgery to be assessed (Pascarella et al. 2011).
Evaluation and Rationale for including selected studies
This study set out to review and evaluate the existing literature on patellar tendinopathy. To evaluate the literature, two measures were taken and scored: the Modified Coleman Methodology Score (mCMS) used for all included studies, and the Methodological Index for Non-Randomized Studies (MINORS) used especially for evaluating bias in the non-randomized studies included for review.
Modified Coleman Methodology Scores (mCMS) were calculated for each article, evaluating ten criteria on an overall scale from 0-100 (Coleman et al. 2000). A score of 100 indicates that the study controlled against various biases and likely avoids chance and confounding. Appendix Table 2 outlines the mCMS criteria used in this review. Studies were independently reviewed by two authors with disputes on scoring settled by a third author as needed. Studies were then ranked based on score being converted to qualitative attributes with poor quality being a score less than 55, fair quality being a score between 55 and 70, good quality being a score between 70 and 85, and excellent quality being a score 85 and 100.
Methodological Index for Non-Randomized Studies (MINORS) criteria was developed in 2003 by Slim et al. and has shown efficacy and validity in assessing the methodology of non-randomized studies (Slim et al. 2003). It is scored on a scale from 0-16 where a score of 16 indicates strong methodology with lower risk of bias. Three categories of quality exist, with a score less than 8 being low quality, a score ranging 8 to 12 being intermediate quality and a score greater than 12 being high quality.
While non-randomized studies are prone to higher risks of bias, the present review was set with restrictions to include solely all prospective studies or RCTs, allowing for decreased bias in the studies included while being able to examine a wide breadth of studies examining arthroscopic patellar tendinopathy outcomes. A table with further considerations for inclusion of non-randomized studies is provided in Table 2.
Data Acquisition and Analysis
Data extraction was conducted manually by performing a full-text review of included studies and stored in Microsoft Excel (Microsoft Corporation. Redmond, WA. 2018). The following data was extracted: study design, study size, male:female ratio, sport at time of injury, duration of symptoms, pre-operative Blazina score, conservative treatment duration, time at last follow-up, surgical technique specifics, post-operative rehabilitation or immobilization, patient-reported outcome measures (PROMs) including VISA-P, Lysholm, VAS scores, reported success rate (%), RTS rate (% as defined by return to same level, or similar level of activity with only minor limitations), average return to sport (RTS) time, and post-operative complications. Success as a category in this review was left as “subjective success” due to differences in definition of success across studies. RTS was defined as the time required for patients to return to their baseline physical activity of choice following surgery. For missing data such as standard deviations of patient-reported outcomes, efforts were made to gather the needed data for analysis from authors of the studies being reviewed.
Studies commonly reported use of the following operative interventions: patellar bony work (PBW), Hoffa’s fat pad debridement (HFPD), denervation of the patella and peripatellar soft tissue (DNRV), as well as post-operative immobilization (POI). Studies could then be coded based on the convention (PBW, HFPD, DNRV, POI). “POI” has been omitted from notation from all other studies due to no other studies utilizing post-operative immobilization.
Statistical analysis was avoided due to heterogeneity of study methodology, and differences in surgical techniques. Confidence intervals (CI) were generated using Clopper-Pearson Single Proportion 95% CI estimations. Data analysis was performed using STATA 14 (StataCorp. College Station, TX. 2015.). PROM scores that were given post-operatively but not recorded pre-operatively were not included in analysis.
Results
Of 72 full-text studies assessed, 64 were excluded yielding a final eight studies included for final analysis, one RCT and seven prospective cohort studies. A summary of each paper can be found in Appendix Table 3.
Study Operative Factors
Two studies were classified as (+PBW +HFPD -DNRV +POI) (Andonovski, Andonovska, and Trpeski 2020; Alaseirlis 2012), two were (+PBW +HFPD -DNRV) (Lee et al. 2018; Pascarella et al. 2011), one was (-PBW +HFPD +DNRV) (Maier et al. 2013), two were (-PBW -HFPD +DNRV) (Pestka et al. 2018; Willberg et al. 2011), and one was (-PBW -HFPD -DNRV) in which the only reported intervention was shaving of the dorsal aspect of the tendon (Willberg et al. 2007). The two studies that implemented POI were Andonovski et al (three weeks) and Alaseirlis et al (three-four weeks) (+PBW +HFPD -DNRV +POI) indicating bony work, Hoffa’s fat pad debridement, and post-operative immobilization, but no denervation (Andonovski, Andonovska, and Trpeski 2020; Alaseirlis et al. 2013).
Quality of Included Studies
The average mCMS for all included studies was 76.4 ± 6.6, which may be categorized as “good” (Table 3). A common deduction of points was in the Assessment of Outcomes category, primarily from lack of an investigator independent of the surgeon, or from lack of clarity regarding if the patient filled out the assessment with “minimal or no help from the reviewer.” The lowest rated studies included in this review suffered a compounding effect of missing points in both aforementioned areas.
The average MINORS score for the seven included non-randomized studies was 11.1 ± 1.1, which would fall into the “intermediate quality” category (Table 4). The most frequent deduction of points according to the MINORS criteria was that all studies lacked a “prospective calculation on cohort size” and were at times ambiguous on patient selection and whether it was “continuous selection” or without certain exclusions. These deductions may expose the studies to increased risk of bias, yet they are still deemed to be of “intermediate quality.”
Success and Return to Sport
A total of 260 patients with a mean follow-up of 45.2 months (range 6-79) were included. One study reported follow-up as a minimum of six months without further specification.
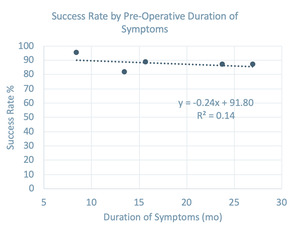
Average success and return to sport (RTS) rates were 90.2% (range 80-100%) and 90.6% (range 85.7-100%), respectively. One study reported complications (failed tendon release) (Pestka et al. 2018). There was a weak negative correlation between reported subjective success rate and pre-operative duration of symptoms (R2=0.14) demonstrated in Figure 2. It was suggested this relationship may be mediated by Hoffa edema of the knee joint (Pestka et al. 2018).
Figure 3 includes forest plots of the study data as it relates to RTS time (range 2.2 months – 4.96 months), RTS rate, and subjective success rates for the patients in each study. Willberg et al. had the most rapid return to sport time with athletes returning to sport on average of 2.2 months post-operatively (Figure 3a). Pestka et al. reported a median of three months (range 0.5-12), and an estimate of 4.66 (95% CI 3.77 – 5.55) was calculated and included by the methods outlined by Hozo et al. (Hozo, Djulbegovic, and Hozo 2005). RTS rate ranged from 86% to 100%, with Alaseirlis et al. and Willberg et al. both reporting all the participants being able to return to sport (Figure 3b). Subjective success rates ranged between 80% and 100% with Pestka et al. reporting 100% success as defined as significant improvement in the VISA-P score post-operatively (Figure 3c). The lowest reported success rate of 80% was from Maier et al in which success was defined as patients rating their knee function as either “good” or “excellent”.
Willberg et al. conducted a randomized control trial comparing arthroscopic patellar denervation (-PBW -HFPD +DNRV) to ultrasound guided sclerosing injections (Willberg et al. 2011). These interventions resulted in success rates of 87% and 53%, respectively. Arthroscopic patients reportedly had a shorter timeline for returning to sport compared to injections due to one-step intervention (Willberg et al. 2011) that excluded bony patellar work and fat pad debridement.
In Maier et al., the original authors did not define specific “success” criteria but reported 80% of their patients having either “excellent” or “good” subjective knee function, and even in those with lower functional ratings it was said that all patients had an increase in function at mean 52.8 ± 36 months follow-up (Maier et al. 2013).
Patient-Reported Outcome Measures
Out of all patient-reported outcome measures, VISA-P was the most widely reported. Forest plots summarizing commonly reported PROMs are reported in Figure 4. All studies reported mean improvement in the PROMs. VISA-P improvement ranged from 34.5 to 45.6 points (Figure 4a). Lysholm score improvement was similar and ranged from 40.0 to 43.5 points. Both VISA-P and Lysholm are on 100-point scales. Visual Analog Scale for pain (VAS) was reported in several studies with arthroscopic interventions with average pain improvement ranging from 5.10 to 6.37 points on a 10-point scale. Willberg et al. also included a non-operative group in which patients received 2mL of sclerosing polidocanol injections to the proximal tendon under US guidance, this provided an average of only 2.79 points of VAS pain improvement.
Willberg et al. demonstrated a statistically significant difference in post-intervention VAS pain scores between the arthroscopic (-PBW -HFPD +DNRV) and injection groups at rest (5±8.3 vs 19.2±23.2, p=0.004) and after activity (12.8±19.3 vs 41.1±28.5, p=0.001) (Willberg et al. 2011).
Additional Measures
In a select group of 29 knees, Pascarella et al. (+PBW +HFPD -DNRV) also reported 10-year follow-up results. Objective measures had decreased by not more than 2.5 points on 100-point scales compared to three years and were still significantly higher than pre-operative scores (p<0.01) (Pascarella et al. 2011).
Lee et al (+PBW +HFPD -DNRV) examined functional and anthropometric results including extensor peak torque at 60º/s and limb symmetry index at mean 51.3 months (Lee et al. 2018). Both measures were significantly improved from 178.2 ± 42.9Nm/kg to 275 ± 39.4Nm/kg and 71.4 ± 19.6% to 92.7 ± 21.7%, respectively (p<0.001).
Discussion
A major finding of this review of prospective studies is that arthroscopic management of refractory patellar tendinopathy leads to a high success rate and rapid RTS. Additional findings are that patellar bony work and Hoffa’s fat pad debridement may not result in quicker RTS and better post-operative outcomes compared to more conservative approaches. This study adds to the exisiting literature by providing a more comprehensive review of the various surgical techniques while examining a larger variety of outcomes such as RTS, success rates, and patient-reported outcomes.
This study reiterates previous studies that suggest arthroscopic approaches for PT may be favorable for athletes or other individuals desiring quick recovery and a low complication rate (Brockmeyer et al. 2015; Cognetti et al. 2023; Everhart et al. 2017). Despite a high RTS rate reported in many studies, athletes may still be at risk of requiring sporting limitations due to symptoms reoccurring past initial follow-up period, as described for 13% of patients in Lee et al. There also may be evidence that some variability in recovery time exists based on which structures are assessed intraoperatively. Most notably, Willberg et al. (-PBW -HFPD -DNRV) patients exhibit a faster RTS (2.2 months) than all other studies, (range 3.0 – 5.0 months). This may support that performing more conservative procedures and avoiding patellar bony work and Hoffa’s fat pad debridement may introduce less iatrogenic damage and require less intense rehabilitation, pending patients do not have a specific indication for PBW or HFPD (Villardi et al. 2019).
Van Rijn et al. examined patellar tendinopathy treated with extracorporeal shockwave therapy (ESWT) and found that a longer duration of symptoms decreased chances of clinical improvement.(van Rijn et al. 2019) This trended towards significance as part of a multivariable model which included older age, and higher hours of training per week. In contrast, Maffulli et al studied revision surgeries for persistent patellar tendinopathy with an open approach and established no significant relationship between DOS and surgical outcomes (Maffulli et al. 2021). In the present study, no significant relationship can be observed between duration of symptoms and subjective success rate. Therefore, no specific amount of time after symptom onset should motivate providers to intervene surgically, and the decision to operate should instead continue to be influenced by persistent failure of conservative measures.
Three common techniques utilized in the arthroscopic treatment of patellar tendinopathy were identified in this review: patellar bony work, debridement of Hoffa’s fat pad, and denervation of the patella. Although frequently used in practice, there is no consensus on which of these interventions are required for success. In prior studies, the stance on any patellar bony work has been equivocal. Kaeding et al. stated that PBW led to improved RTS rates but similar RTS time to those without PBW, and slightly lower success rates (Kaeding, Pedroza, and Powers 2007). Subsequent reviews have mentioned the potential impact of PBW but have been unable to conclude if it is more beneficial or harmful (Brockmeyer et al. 2015; Cognetti et al. 2023). The studies included in this review that conducted PBW reported significant increases in PROMs from the pre- to postoperative period (Lee et al. 2018; Andonovski, Andonovska, and Trpeski 2020; Alaseirlis 2012; Pascarella et al. 2011). Significant increases in PROMs were also reported in the studies that did not conduct PBW (Maier et al. 2013; Pestka et al. 2018; Willberg et al. 2011). Further prospective studies controlling for patient demographics, imaging findings, and postoperative rehabilitation protocols are required to determine the isolated impact of patellar bony procedures on outcomes.
Debridement of Hoffa’s fat pad is thought to help reduce pathologic edema, which may be a risk factor for failing nonoperative management (Cognetti et al. 2023; Williams et al. 2017). Given the proximity and relative ease of attempting a Hoffa’s pad debridement during a dorsal PT debridement, its efficacy should be further studied in isolation during a randomized control trial.
Denervation of the patella through ligation or cauterization of peripatellar soft tissue may lead to desensitization of anterior knee pain in patients with patellofemoral pathologies (Vega, Golanó, and Pérez-Carro 2006; Wojtys et al. 1990). This review included three studies that conducted denervation as part of arthroscopic treatment which reported no major complications and high success rates ranging from 80 – 100% (Maier et al. 2013; Pestka et al. 2018; Willberg et al. 2011).
Willberg et. al conducted a randomized control trial comparing US-guided arthroscopic shaving of dorsal extratendinous neovessels and nerves (-PBW -HFPD +DNRV) to a control group of polidocanol injections (Willberg et al. 2011). The arthroscopic treatment group had significantly higher success rates and reduction in pain, and patients were allowed to return to full loading activity at two weeks. This resulted in a significantly faster RTS time, although the mean difference was not reported. This study built upon previous articles that emphasized the efficacy and safety of patellar denervation and highlighted an ability to accelerate recovery times compared to intratendinous procedures (Alfredson and Ohberg 2005; Hoksrud et al. 2006).
Immobilization of the knee joint post-operatively was once common practice, but in the last few decades has largely been replaced by early motion to enhance healing supposedly through increased blood flow (Leadbetter et al. 1992; Martens et al. 1982). The present review suggests that immobilization has a variable impact on patient outcomes, including a slightly lower perception of the surgery as a “success” despite significantly improved objective measures and marginally faster return to sport times. This is somewhat consistent with a prior review by Kaeding et al. in which they found immobilized patients to have lower success rates compared to patients who received early motion during rehabilitation (82.4% vs 94.9%) (Kaeding, Pedroza, and Powers 2007), but no measure of significance was reported. The use of immobilization should be further investigated and remains dependent on surgeon and patient preference in patients who require patellar bony work.
In the future, a large-scale RCT comparing individual interventions (i.e. +/-PBW and +/- POI, +/- HFPD, and +/- DNRV) would provide valuable data that would more properly assess impact of these techniques given similar pre- and postoperative management of arthroscopic patellar tendinopathy patients. Additionally, future studies should include multiple PROMs to allow for stronger pooled analysis and account for the inability of any specific measure to perfectly characterize clinically perceptible differences (Hernandez-Sanchez, Hidalgo, and Gomez 2014; Korakakis et al. 2021).
Limitations
The results of the present review are limited to the scope of published prospective studies on outcomes following arthroscopic management of patellar tendinopathy. Of the eight studies meeting inclusion criteria, most lack control groups for comparison, and variability in intervention, post-operative management, and assessment tools and activity scores limit the ability to meta-analyze the data (Dan et al. 2019; Brockmeyer et al. 2015; Kaeding, Pedroza, and Powers 2007).
Further, mean follow-up times for included studies ranged from 6-79 months, impairing the ability to compare long-term outcomes of each variable examined in the study. Patients may have relapsed in their symptoms after most recent recorded follow-ups, impairing the ability to make conclusions on the permanence of relief from different arthroscopic interventions. A minimum follow-up of six months further limits the number of studies that could be included in this review.
Additionally, slight variations in the definition of success among papers and among patients likely impact the reliability of using success rate to identify superior or inferior practices. Validated PROMs such as the VISA-P score were not reported in all studies included despite being a relatively reliable assessment tool. Also, none of the included studies utilized patient reported improvement tools, such as minimal clinically important difference (MCID) or patient acceptable symptom state (PASS), which can provide more in depth information about the efficacy of surgery from the patient perspective.
Lastly, there was great heterogeneity amongst the studies with an average MINORS criteria score of intermediate quality, potentially lowering the strength of conclusions from the synthesis of data.
Conclusions
For refractory patellar tendinopathy, arthroscopic debridement of the patellar tendon is a safe and effective procedure that allows rapid return to sport. Surgeons may elect to forgo patellar bony work and Hoffa’s fat pad debridement in favor of a conservative approach for athletes seeking to return to sport quickly. However, these decisions should always be considered in the circumstances of the individual patient and intraoperative findings.
Author Contributions
CV: Writing- original draft and revision and editing, investigation; JO: Conceptualization, investigation; GB: Conceptualization, writing-original draft and revision and editing, formal analysis, investigation; YA: writing – revision and editing; EM: Supervision, investigation; PC: Supervision, revision of manuscript; RD: Conceptualization, supervision; RM: Conceptualization, supervision; CK: conceptualization, supervision; DF: conceptualization, supervision.
Legend For Figures
Figure 3. Forest plots depicting the reported means and 95% confidence intervals for (a.) Return to Sport time in months (RTS time), (b.) Percentage of players able to return to sport (RTS %) (c.) Percentage of patients with subjective success .
Figure 4. Forest plots depicting the reported means and 95% confidence intervals for post-operative improvements in (a.) Victorian Institute of Sports Assessment patellar tendon (VISA-P), (b.) Lysholm and (c.) Visual Analog Scale (VAS) pain scores.